What Is A Tailor'S Bunion?
Overview
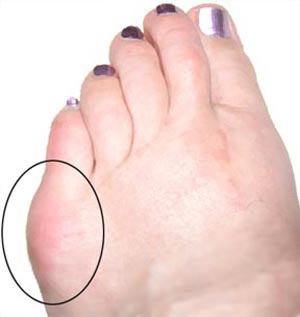 Bunion is the common term for a medical condition known as Hallux Valgus. Hallux Valgus is the tilting of the toe away from the mid-line of the body. It is usually characterized by a lump or bump that is red, swollen and/or painful on the inside of the foot in and around the big toe joint.
Bunion is the common term for a medical condition known as Hallux Valgus. Hallux Valgus is the tilting of the toe away from the mid-line of the body. It is usually characterized by a lump or bump that is red, swollen and/or painful on the inside of the foot in and around the big toe joint.
Causes
Bunions are most widely considered to be due to an imbalance in the forces that is exerted across the joint during walking. The resulting abnormal motion and pressure over the joint, over many years (combined with poor fitting footwear) leads to instability in the joint causing hallux valgus and bunions. Bunions are really only a symptom of faulty foot mechanics and are usually caused by a combination of the way we walk, the foot we inherit and inappropriate footwear use.
Symptoms
Look for an angular, bony bump on the side of the foot at the base of the big toe. Sometimes hardened skin or a callus covers this bump. There's often swelling, redness, unusual tenderness, or pain at the base of the big toe and in the ball of the foot. Eventually, the area becomes shiny and warm to the touch. Seek medical advice if you have persistent pain when walking normally in otherwise comfortable, flat-soled shoes, you may be developing a bunion, bursitis, or a bone spur in your foot.
Diagnosis
Before examining your foot, the doctor will ask you about the types of shoes you wear and how often you wear them. He or she also will ask if anyone else in your family has had bunions or if you have had any previous injury to the foot. In most cases, your doctor can diagnose a bunion just by examining your foot. During this exam, you will be asked to move your big toe up and down to see if you can move it as much as you should be able to. The doctor also will look for signs of redness and swelling and ask if the area is painful. Your doctor may want to order X-rays of the foot to check for other causes of pain, to determine whether there is significant arthritis and to see if the bones are aligned properly.
Non Surgical Treatment
Treatment may be surgical or non-surgical. The goal of non-surgical treatment is to relieve pressure on the foot and to prevent pressure sores and foot ulcers. This is accomplished by prescribing accommodative shoes with a wide toe box - sandals or extra depth shoes with soft moulded insoles. It may also be possible to relax the leather on shoes to make room for a bunion. 
Surgical Treatment
Sometimes a screw is placed in the foot to hold a bone in a corrected position, other times a pin, wire or plate is chosen. There are even absorbable pins and screws, which are used for some patients. In British Columbia, pins seem to be used most frequently, as they're easier to insert and less expensive. They are typically--but not always--removed at some point in the healing process. But as a general rule, Dr. Schumacher prefers to use screws whenever possible, as they offer some advantages over pins. First, using screws allows you to close over the wound completely, without leaving a pin sticking out of the foot. That allows for a lower infection rate, it allows you to get your foot wet more quickly following the surgery, and it usually allows for a quicker return to normal shoes. Second, they're more stable than pins and wires. Stability allows for faster, more uneventful, bone healing. Third, they usually don't need to be removed down the road, so there's one less procedure involved.
What Does Over-Pronation Mean
You know when we walk in the sand on the beach? Well, that?s how nature meant us to walk! You will notice how the sand forms a complete support under the foot. Unfortunately, instead of soft natural surfaces, we walk mainly on hard surfaces like pavements and floors. These hard surfaces cause the foot to roll inwards and the arches to flatten to gain ground contact. This condition is called ?over-pronation? and it affects an estimated 70% of the population. Over-pronation can lead to various foot problems such as heel pain and ball of foot pain. Because our feet are the foundation of our body, poorly aligned feet may also cause problems in other parts of the body, resulting in shin pain, aching legs, knee pain, even lower back pain.

Causes
There has been some speculation as to whether arch height has an effect on pronation. After conducting a study at the Rose-Hulman Institute of Technology, Maggie Boozer suggests that people with higher arches tend to pronate to a greater degree. However, the generally accepted view by professionals is that the most pronation is present in those with lower arch heights. To complicate matters, one study done by Hylton Menz at the University of Western Sydney-Macarthur suggests that the methods for measuring arch height and determining whether someone is ?flat-footed? or ?high-arched? are unreliable. He says, ?For this reason, studies investigating the relationship between static arch height motion of the rearfoot have consistently found that such a classification system is a poor predictor of dynamic rearfoot function.
Symptoms
Overpronation can lead to injuries and pain in the foot, ankle, knee, or hip. Overpronation puts extra stress on all the bones in the feet. The repeated stress on the knees, shins, thighs, and pelvis puts additional stress on the muscles, tendons, and ligaments of the lower leg. This can put the knee, hip, and back out of alignment, and it can become very painful.
Diagnosis
When you overpronate your foot rolls inwards causing the lower leg to rotate inwards too. It's thought that this increases stress on the soft tissues of the lower leg causing pain and inflammation, or more commonly known as shin splints.

Non Surgical Treatment
Side Step with Opposite Reach. This exercise is designed to load the "bungee cord system" of the gluteal muscle and its opposite, latissimus dorsi muscle to keep the foot from overpronating. Because the opposite arm swings across the front leg when walking, this exercise creates tension in the muscles all the way from the front foot, across the back of the hips and back, to the fingers of the opposite hand. Movement Directions. Stand with left foot on top of the dome of the BT. (Note: For added balance, the right foot can tap on the ground, if needed). Reach right leg out to the side of the BT, and tap the ground while squatting down on the left side and reaching right arm across the left knee. Push down with left big toe while squatting. This activates the arch of the left foot and strengthens all the stabilizing muscles on the left side of the lower body. Return to starting position. Perform 8 to 10 repetitions on each leg.
Prevention
Massage and stretch the calves to increase dorsiflexion at the foot/ankle. Dorsiflexion is the bending at the ankle. By improving the dorsiflexion, one will have more flexibility at the ankle, which will allow the foot to over-pronate less. Massage the IT Band with a foam roller or tennis ball to quiet down the tightness throughout this part of the leg. The IT Band attaches from the glute maximus and runs down the side of the leg into the knee area. When the IT Band is tight it will accelerate the force of the leg moving inward, which will cause the foot to move inward as well. It is often that tightness through the IT Band that promotes over-pronation. Decreasing over-pronation, which is very prominent in runners, will help add endurance, speed and efficiency to your run and ultimately place less stress on your body.
Rehab For Calcaneal Apophysitis
Sever?s disease is the most common cause of heel pain in children aged 9 to 14. Sever?s disease results from stress placed on the growth plate of the heel bone. An excessive amount of running or other activities can cause inflammation around the growth plate, which results in pain. Rest, ice and orthotics and proper shoes are usually prescribed.
Causes
Growth plates, also called epiphyseal plates, occur at the end of long bones in children who are still growing. These plates are at either end of growing bones, and are the place where cartilage turns into bone. As children grow, these plates eventually become bone (a process called ossification). During a growth spurt, the bone in the heel may outpace the growth of the muscles and tendons that are attached to the heel, such as the Achilles tendon. During weight bearing, the muscles and tendons begin to tighten, which in turn puts stress on the growth plate in the heel. The heel is not very flexible, and the constant pressure on it begins to cause the symptoms of Sever?s disease. Sever?s disease is common, and it does not predispose a child to develop any other diseases or conditions in the leg, foot, or heel. It typically resolves on its own.
Symptoms
Pain is usually felt at the back of the heel and around the sides of the heel. If you squeeze the back of the heel from both sides simultaneously and pain is experienced Sever?s disease is more than likely present.
Diagnosis
A doctor can usually tell that a child has Sever's disease based on the symptoms reported. To confirm the diagnosis, the doctor will probably examine the heels and ask about the child's activity level and participation in sports. The doctor might also use the squeeze test, squeezing the back part of the heel from both sides at the same time to see if doing so causes pain. The doctor might also ask the child to stand on tiptoes to see if that position causes pain. Although imaging tests such as X-rays generally are not that helpful in diagnosing Sever's disease, some doctors order them to rule out other problems, such as fractures. Sever's disease cannot be seen on an X-ray.
Non Surgical Treatment
Treatment may consist of one or more of the following. Elevating the heel. Stretching hamstring and calf muscles 2-3 times daily. Using R.I.C.E. (Rest, Ice, Compression, Elevation). Foot orthotics. Medication. Physical therapy. Icing daily (morning). Heating therapy. Open back shoe are best and avoid high heel shoe. The Strickland Protocol has shown a positive response in patients with a mean return to sport in less than 3 weeks. Further research into the anatomical and biomechanical responses of this protocol are currently being undertaken.
What Is Posterior Tibial Tendon Dysfunction
Overview
Adult Acquired Flatfoot (Posterior Tibial Tendon Dysfunction) is a painful, progressive deformity in adults. It results from a gradual stretch (attenuation) of the tibialis posterior tendon and the ligaments that support your foot?s arch. This stretching causes the tendon to lose strength and function. Many people have flat feet and do not experience pain. However, pain occurs with Adult Acquired Flatfoot because the tendons and ligaments have been torn. Once the vital ligaments and posterior tibial tendon are lost, there is no longer anything holding the arch of the foot in place. 
Causes
Damage to the posterior tendon from overuse is the most common cause for adult acquired flatfoot. Running, walking, hiking, and climbing stairs are activities that add stress to this tendon, and this overuse can lead to damage. Obesity, previous ankle surgery or trauma, diabetes (Charcot foot), and rheumatoid arthritis are other common risk factors.
Symptoms
Often, this condition is only present in one foot, but it can affect both. Adult acquired flatfoot symptoms vary, but can swelling of the foot's inner side and aching heel and arch pain. Some patients experience no pain, but others may experience severe pain. Symptoms may increase during long periods of standing, resulting in fatigue. Symptoms may change over time as the condition worsens. The pain may move to the foot's outer side, and some patients may develop arthritis in the ankle and foot.
Diagnosis
In diagnosing flatfoot, the foot & Ankle surgeon examines the foot and observes how it looks when you stand and sit. Weight bearing x-rays are used to determine the severity of the disorder. Advanced imaging, such as magnetic resonance imaging (MRI) and computed tomography (CAT or CT) scans may be used to assess different ligaments, tendons and joint/cartilage damage. The foot & Ankle Institute has three extremity MRI?s on site at our Des Plaines, Highland Park, and Lincoln Park locations. These extremity MRI?s only take about 30 minutes for the study and only requires the patient put their foot into a painless machine avoiding the uncomfortable Claustrophobia that some MRI devices create.
Non surgical Treatment
Because of the progressive nature of PTTD, early treatment is advised. If treated early enough, your symptoms may resolve without the need for surgery and progression of your condition can be arrested. In contrast, untreated PTTD could leave you with an extremely flat foot, painful arthritis in the foot and ankle, and increasing limitations on walking, running, or other activities. In many cases of PTTD, treatment can begin with non-surgical approaches that may include. Orthotic devices or bracing. To give your arch the support it needs, your foot and ankle surgeon may provide you with an ankle brace or a custom orthotic device that fits into the shoe. Immobilization. Sometimes a short-leg cast or boot is worn to immobilize the foot and allow the tendon to heal, or you may need to completely avoid all weight-bearing for a while. Physical therapy. Ultrasound therapy and exercises may help rehabilitate the tendon and muscle following immobilization. Medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, help reduce the pain and inflammation. Shoe modifications. Your foot and ankle surgeon may advise changes to make with your shoes and may provide special inserts designed to improve arch support. 
Surgical Treatment
Stage two deformities are less responsive to conservative therapies that can be effective in mild deformities. Bone procedures are necessary at this stage in order to recreate the arch and stabilize the foot. These procedures include isolated fusion procedures, bone grafts, and/or the repositioning of bones through cuts called osteotomies. The realigned bones are generally held in place with screws, pins, plates, or staples while the bone heals. A tendon transfer may or may not be utilized depending on the condition of the posterior tibial tendon. Stage three deformities are better treated with surgical correction, in healthy patients. Patients that are unable to tolerate surgery or the prolonged healing period are better served with either arch supports known as orthotics or bracing such as the Richie Brace. Surgical correction at this stage usually requires fusion procedures such as a triple or double arthrodesis. This involves fusing the two or three major bones in the back of the foot together with screws or pins. The most common joints fused together are the subtalar joint, talonavicular joint, and the calcaneocuboid joint. By fusing the bones together the surgeon is able to correct structural deformity and alleviate arthritic pain. Tendon transfer procedures are usually not beneficial at this stage. Stage four deformities are treated similarly but with the addition of fusing the ankle joint.
What Can Cause Heel Serious Pain

The heel is a cushion of fatty tissue that protects the structures of the foot, including the heel bone, muscles and ligaments. Heel Pain is a common foot complaint. Complications include plantar fasciitis and heel spurs. Sever's disease is a common cause of heel pain in children. A podiatrist can help diagnose and treat heel pain. The heel is a padded cushion of fatty tissue around the heel bone (the calcaneus) that holds its shape despite the pressure of body weight and movement. It serves to protect the structures of the foot, including the calcaneus, muscles and ligaments. Heel pain is a very common foot complaint. Anyone can suffer from heel pain, but certain groups seem to be at increased risk, including, middle-aged men and women, physically active people, people who are overweight or obese, people who are on their feet for long periods of time, children aged between eight and 13 years (particularly boys) and women during pregnancy.
Causes
A sharp stabbing pain, like a nail going into the bottom of the heel when first stepping on the foot after getting out of bed or after sitting for period of time, is the most common description for plantar fasciitis or heel spur syndrome. Typically the pain eases off as the day goes on but it may not go away completely. A thick ligament that attaches to the bottom of the heel and runs the length of the foot to the toes can become inflamed and swollen at the attachment site. This tends to be an overuse type of injury where poor foot structure is involved; also, wearing of shoe gear that lacks adequate support (ie: worn out shoes, boots and flip-flops) and prolonged standing or walking are often implicated. A throbbing pain that gets worse as the day goes on and can be worse at night when laying in bed is most often associated with an irritated or entrapped nerve on the inside of the ankle or heel. This is similar to carpel tunnel syndrome in the wrist and hand. Approximately 7 / 10 patients with heel pain have a component of nerve entrapment as the cause of their heel pain. This is also one of the most common causes of chronic heel pain because it is often missed as a diagnosis. When nerve entrapment is considered to be a cause, painless neurosensory testing is performed with the Pressure Specified Sensory Device? (PSSD) at The Foot & Ankle Center, PC to determine the extent of compression. A less common cause of heel pain but a stress fracture is often considered in athletes, such as long distance runners, who have heel pain. Posterior Heel Pain (Retrocalcaneal) This is pain in the back of the heel that flares up when first starting an activity. It is often associated with a large bump that can be irritated by shoes. The Achilles tendon attaches to the back of the heel and, like on the bottom, this attachment site can often become inflamed; a spur may or may not be present. Another painful area is a sac of fluid (bursa) that sits between the tendon and bone to act as a cushion for the tendon. This bursa can become inflamed often leading to significant pain called retrocalcaneal bursitis.
Symptoms
Depending on the specific form of heel pain, symptoms may vary. Pain stemming from plantar fasciitis or heel spurs is particularly acute following periods of rest, whether it is after getting out of bed in the morning, or getting up after a long period of sitting. In many cases, pain subsides during activity as injured tissue adjusts to damage, but can return again with prolonged activity or when excessive pressure is applied to the affected area. Extended periods of activity and/or strain of the foot can increase pain and inflammation in the foot. In addition to pain, heel conditions can also generate swelling, bruising, and redness. The foot may also be hot to the touch, experience tingling, or numbness depending on the condition.
Diagnosis
In most cases, your GP or a podiatrist (a specialist in foot problems and foot care) should be able to diagnose the cause of your heel pain by asking about your symptoms and medical history, examining your heel and foot.
Non Surgical Treatment
Heel pain often goes away on its own with home care. For heel pain that isn't severe, try the following. Rest. If possible, avoid activities that put stress on your heels, such as running, standing for long periods or walking on hard surfaces. Ice. Place an ice pack or bag of frozen peas on your heel for 15 to 20 minutes three times a day. New shoes. Be sure your shoes fit properly and provide plenty of support. If you're an athlete, choose shoes appropriate for your sport and replace them regularly. Foot supports. Heel cups or wedges that you buy in the drugstore often provide relief. Custom-made orthotics usually aren't needed for heel problems. Over-the-counter pain medications. Aspirin or ibuprofen (Advil, Motrin IB, others) can reduce inflammation and pain.
Surgical Treatment
At most 95% of heel pain can be treated without surgery. A very low percentage of people really need to have surgery on the heel. It is a biomechanical problem and it?s very imperative that you not only get evaluated, but receive care immediately. Having heel pain is like having a problem with your eyes; as you would get glasses to correct your eyes, you should look into orthotics to correct your foot. Orthotics are sort of like glasses for the feet. They correct and realign the foot to put them into neutral or normal position to really prevent heel pain, and many other foot issues. Whether it be bunions, hammertoes, neuromas, or even ankle instability, a custom orthotic is something worth considering.
Prevention

Being overweight can place excess pressure and strain on your feet, particularly on your heels. Losing weight, and maintaining a healthy weight by combining regular exercise with a healthy, balanced diet, can be beneficial for your feet. Wearing appropriate footwear is also important. Ideally, you should wear shoes with a low to moderate heel that supports and cushions your arches and heels. Avoid wearing shoes with no heels.
Achilles Tendonitis Treatment And Cause
 Achilles tendinitis can be a very crippling issue for runners - simply because the pain is enough to discourage loading of the foot. It can also be a tricky condition to treat because the tendon is not as heavily vascularized (i.e. more blood flow) as muscle, and therefore lacks healing potential. It is highly recommended that you see a physical therapist as soon as you experience acute symptoms, so chronic tendonosis (which is longer termed and harder to treat) does not set in.
Achilles tendinitis can be a very crippling issue for runners - simply because the pain is enough to discourage loading of the foot. It can also be a tricky condition to treat because the tendon is not as heavily vascularized (i.e. more blood flow) as muscle, and therefore lacks healing potential. It is highly recommended that you see a physical therapist as soon as you experience acute symptoms, so chronic tendonosis (which is longer termed and harder to treat) does not set in.
Causes
There are a number of causes and risk factors associated with Achilles Tendinitis. One of the most common causes is simply a lack of conditioning. If the tendon, and muscles that connect to the tendon, have not been trained or conditioned, this can lead to a weakness that may result in an Achilles injury. Overtraining is also associated with Achilles Tendinitis. Doing too much, too soon places excessive strain on the Achilles tendon and doesn't allow the tendon enough time to recovery properly. Over time small tears and general degeneration result in a weakening of the tendon, which leads to inflammation and pain. Other causes of Achilles injury include a lack of warming up and stretching. Wearing inadequate footwear, running or training on uneven ground, and simply standing on, or in something you're not meant to. Biomechanical problems such as high arched feet or flat feet can also lead to Achilles injuries.
Symptoms
Gradual onset of pain and stiffness over the tendon, which may improve with heat or walking and worsen with strenuous activity. Tenderness of the tendon on palpation. There may also be crepitus and swelling. Pain on active movement of the ankle joint. Ultrasound or MRI may be necessary to differentiate tendonitis from a partial tendon rupture.
Diagnosis
Confirming Achilles tendonitis may involve imaging tests. X-rays provide images of the bones of the foot and leg. Magnetic resonance imaging (MRI) is useful for detecting ruptures and degeneration of tissue. Ultrasound shows tendon movement, related damage, and inflammation.
Nonsurgical Treatment
Treatment for Achilles tendonitis, depends on the severity of the injury. If heel pain, tenderness, swelling, or discomfort in the back of the lower leg occurs, physical activity that produces the symptoms should be discontinued. If the problem returns or persists, a medical professional should be consulted. If pain develops even with proper stretching and training techniques, the patient should consult a podiatrist to check for hyperpronation and adequate arch support. The addition of an orthotic may be enough to maintain good arch and foot alignment and eliminate pain. If damage to the tendon is minor, the injury may respond to a simple course of treatment known as RICE (rest, ice, compression, elevation). Patients are advised to rest the tendon by keeping off their feet as much as possible, apply ice packs for 20 minutes at a time every hour for a day or two to reduce swelling, compress the ankle and foot with a firmly (not tightly) wrapped elastic bandage and elevate the foot whenever possible to minimize swelling. A nonsteroidal anti-inflammatory drug (NSAID) such as ibuprofen may be used to reduce pain, swelling, and inflammation.

Surgical Treatment
If non-surgical approaches fail to restore the tendon to its normal condition, surgery may be necessary. The foot and ankle surgeon will select the best procedure to repair the tendon, based upon the extent of the injury, the patient?s age and activity level, and other factors.
Prevention
A 2014 study looked at the effect of using foot orthotics on the Achilles tendon. The researchers found that running with foot orthotics resulted in a significant decrease in Achilles tendon load compared to running without orthotics. This study indicates that foot orthoses may act to reduce the incidence of chronic Achilles tendon pathologies in runners by reducing stress on the Achilles tendon1. Orthotics seem to reduce load on the Achilles tendon by reducing excessive pronation,
What Triggers Pain Of The Heel And The Way To Cure It

Overview
Heel pain is most commonly caused by plantar fasciitis, which is the swelling of the tissue that connects the heel bone to the toes at the bottom part of the foot, also known as the plantar fascia. Plantar fasciitis is often described as sharp pain in the middle of the heel, which is typically worse after periods of rest when fascia contracts. The pain usually becomes more bearable as the muscles loosen up during the low-impact walking, but can return even worse after extended periods of walking or standing. The plantar fascia serves as a shock absorber and supports the foot’s arch. Too much tension on the plantar fascia can cause inflammation and swelling. Fortunately in most cases, plantar fasciitis treatment is fairly conservative. Plantar fasciitis exercises, medications and orthotics are usually all that’s needed to manage the pain. Most severe cases may require surgery.
Causes
Plantar fasciitis is a painful disorder in the lower part of your foot usually around the heel. That pain usually hurts as you get up in the morning when you try to stand on your feet, or after any periods of inactivity. It is a disorder of a tough and strong band that connects the heel bone to the toes. Plantar Fasciitis is caused by injuring that tough band on the bottom of the foot. The following may be the causes of plantar fasciitis. Tight calf muscles or tight Achilles tendon produces repetitive over-stretching of the plantar fascia. Gait and balance Problem may be a dominant cause of this disorder. Many people have a special style of walking, with something unique that causes some kind of imbalance in their body. It might be something like locked knees, feet that turn-out, a weak abdomen etc. This imbalance may place some pressure on the fascia, which eventually causes plantar fasciitis. Weak foot muscles don’t give enough support to the plantar fascia. The small muscles in the foot give the foot its shape by keeping the bones in place and by expanding and contracting to make a movement. Weak foot muscles will allow greater stress on the fascia. Foot anatomical problems such as flat feet or high arches can make the fascia ligament work or stretch abnormally. Flattening of the fat pad at the sole of the feet under the heels is a Degeneration process that is caused by poor footwear or by age. Shoes that have no proper heel cup can flatten that fat pad quite quickly and cause this disorder. Walking in shoes which do not have good arch support is considered to be a cause of plantar fasciitis. Wearing inadequate or worn out shoes may place more stress on the fascia ligament. If you wear shoes that don't fit you by size or width, you may put your feet under excessive stress. Overweight Men and women are more vulnerable to developing the condition because of the excess weight on the foot. Pregnant women are at risk due to gaining weight through pregnancy and due to the pregnancy hormones that make ligaments loosen and relax. Sudden increase of activity like starting to run long distance or complete change of daily activity can cause heel pain and this disorder. Practice of repetitive athletic activities, like long distance running, playing a ball game, dancing or jumping, is a common cause for the disorder. Actually it is considered as one of the most common running injuries. Spending long periods of time on your feet everyday can cause plantar fasciitis. Working on your feet a few hours a day evey day may be the reason for your heel pain.
Symptoms
Symptoms of plantar fasciitis can occur suddenly or gradually. When they occur suddenly, there is usually intense heel pain on taking the first morning steps, known as first-step pain. This heel pain will often subside as you begin to walk around, but it may return in the late afternoon or evening. When symptoms occur gradually, a more long-lasting form of heel pain will cause you to shorten your stride while running or walking. You also may shift your weight toward the front of the foot, away from the heel.
Diagnosis
Plantar fasciitis is one of many conditions causing "heel pain". Some other possible causes include nerve compression either in the foot or in the back, stress fracture of the calcaneus, and loss of the fatty tissue pad under the heel. Plantar fasciitis can be distinguished from these and other conditions based on a history and examination done by a physician. It should be noted that heel spurs are often inappropriately thought to be the sole cause of heel pain. In fact, heel spurs are common and are nothing more than the bone's response to traction or pulling-type forces from the plantar fascia and other muscles in the foot where they attach to the heel bone. They are commonly present in patients without pain, and frequently absent from those who have pain. It is the rare patient who has a truly enlarged and problematic spur requiring surgery.
Non Surgical Treatment
Treatment for plantar fasciitis includes medication, physical therapy, shock wave therapy, or surgery. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen are used to treat the inflammation and pain of plantar fasciitis, but they won’t cure the condition. Corticosteroids can also be used to ease pain and reduce inflammation. Corticosteroids are applied either as a topical solution in conjunction with a non-painful electric current or through injections to the affected area.

Surgical Treatment
The majority of patients, about 90%, will respond to appropriate non-operative treatment measures over a period of 3-6 months. Surgery is a treatment option for patients with persistent symptoms, but is NOT recommended unless a patient has failed a minimum of 6-9 months of appropriate non-operative treatment. There are a number of reasons why surgery is not immediately entertained including. Non-operative treatment when performed appropriately has a high rate of success. Recovery from any foot surgery often takes longer than patients expect. Complications following this type of surgery can and DO occur! The surgery often does not fully address the underlying reason why the condition occurred therefore the surgery may not be completely effective. Prior to surgical intervention, it is important that the treating physician ensure that the correct diagnosis has been made. This seems self-evident, but there are other potential causes of heel pain. Surgical intervention may include extracorporeal shock wave therapy or endoscopic or open partial plantar fasciectomy.
Prevention
Making sure your ankle, Achilles tendon, and calf muscles are flexible can help prevent plantar fasciitis. Stretch your plantar fascia in the morning before you get out of bed. Doing activities in moderation can also help.